Medical Billing: The Cycle That Never Sleeps
Master revenue cycle management: Optimize billing, cut denials, boost reimbursements & financial health in healthcare.
Master revenue cycle management: Optimize billing, cut denials, boost reimbursements & financial health in healthcare.


Revenue cycle management is the financial engine that keeps healthcare organizations running—tracking every dollar from the moment a patient schedules an appointment until the final payment clears. It encompasses all administrative and clinical functions that contribute to capturing, managing, and collecting patient service revenue.
Quick Overview: What Revenue Cycle Management Includes
The financial stakes are enormous. Claim denials alone cost hospitals roughly $262 billion per year, and providers fail to collect 2-5% of net patient revenue due to inefficient processes. Yet many healthcare practices still treat revenue cycle management as just "billing"—missing critical gaps in registration, coding, follow-up, and collections that delay payment for months.
The reality? Revenue cycle management isn't formally taught in medical residency, leaving clinicians to learn on the job while juggling patient care. Front-desk errors, coding inaccuracies, and inconsistent insurance follow-up create bottlenecks that strangle cash flow. Simply working hard isn't enough to maintain a profitable practice—prompt and complete payment for services is just as critical.
I'm Ryan T. Murphy, founder of UpfrontOps, and over the past 12 years I've helped 32 companies streamline their operations by fixing broken processes, cleaning up messy data, and implementing smart automation—skills that directly translate to optimizing Revenue cycle management workflows. Whether it's reducing denial rates, accelerating collections, or implementing technology that eliminates manual tasks, I've seen how the right systems can unlock millions in revenue that was already earned but never collected.
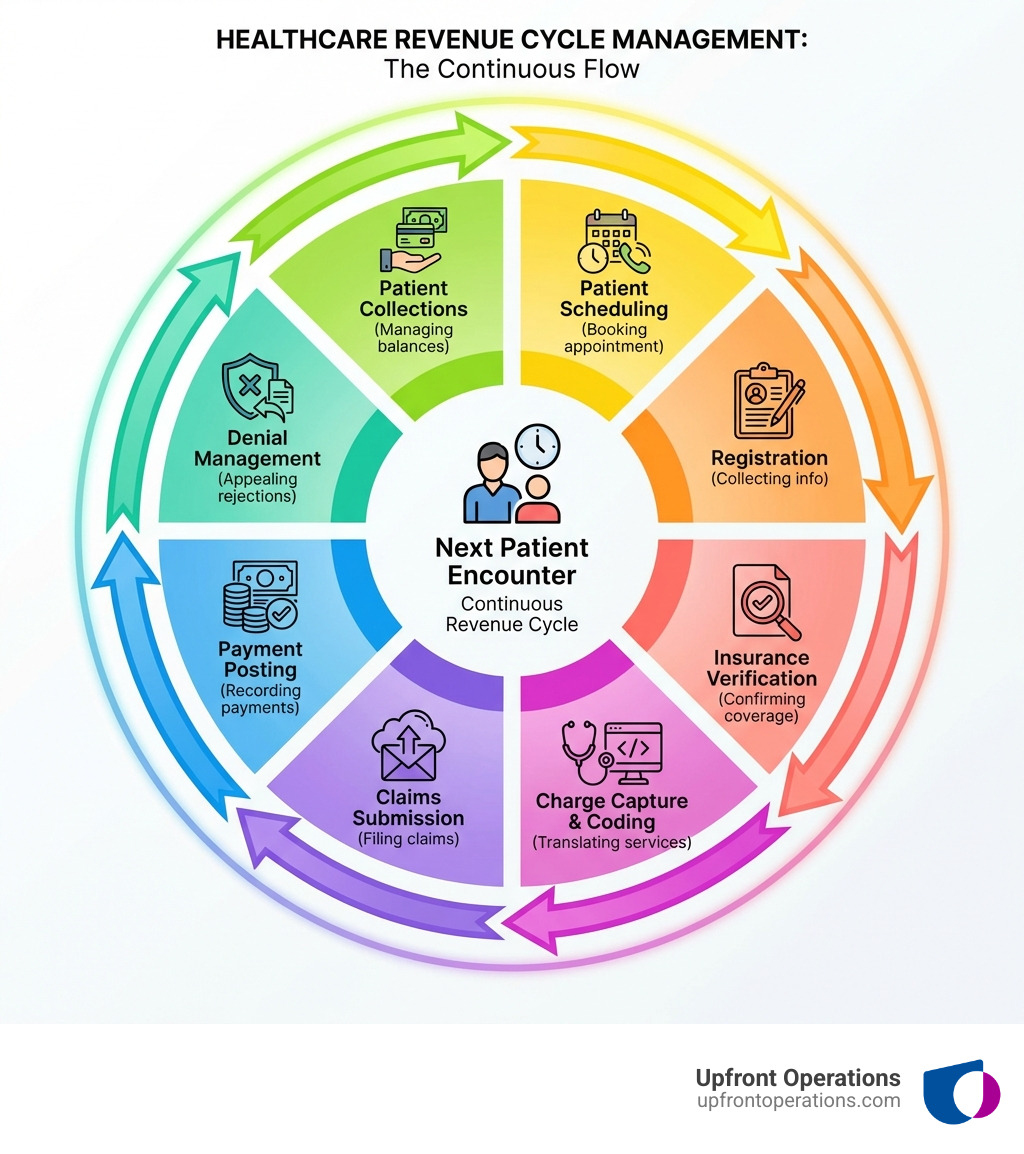
Simple guide to Revenue cycle management:

At its core, Revenue cycle management (RCM) is the process healthcare systems use to track revenue from patients, from their initial appointment to the final payment of a balance. It isn't just a back-office accounting task; it is a complex blend of administrative functions (like scheduling and registration) and clinical functions (like documentation and coding).
In places like New York, where the healthcare market is highly competitive and regulations are tight, maintaining ICD-10 compliance is non-negotiable. RCM teams are responsible for ensuring every clinical interaction is translated into a language that insurance companies understand. When this translation fails, the financial consequences are staggering. Research into claim denial costs shows that the industry loses hundreds of billions annually simply because the "paperwork" didn't match the "procedure" (see this overview of medical claim denial costs).
To manage this, we break the cycle down into eight distinct stages. At Upfront Operations, we believe that whether you are managing a medical practice or a sales pipeline, the principles of flow and accuracy remain the same. If you want operational help you can turn on quickly (without long agency retainers), you can explore our on-demand microservices and fractional support on our services page — from business email setup and website setup to CRM cleanup and pipeline automation.
The cycle actually begins before the patient sees a provider. A consumer-centric approach treats the patient like a valued customer from day one.
Once the patient is in the exam room, the focus shifts to data integrity.
The "back end" of the cycle is where the actual money moves.
| Payer Type | Benchmark: Days to Pay |
|---|---|
| Private Insurance | 12-20 Days |
| Medicare | 18-30 Days |
| Workers' Comp | 55-75 Days |
You cannot manage what you do not measure. In Revenue cycle management, data is the only way to ensure operational efficiency. When you consider that providers fail to collect 2-5% of net patient revenue simply due to inefficient RCM, the need for a "fractional expert" mindset becomes clear.
At Upfront Operations, we help businesses supercharge their CRM and data management. In healthcare, that data management is what prevents your practice from becoming a statistic in that $262 billion annual denial cost. If you're ready to see how elite operational support can scale your momentum, view our pricing.
To keep the financial heart of your practice beating, we monitor these critical KPIs:
Productivity isn't just about working faster; it's about reducing friction.
The "old way" of doing RCM involved stacks of paper and manual data entry. Today, we leverage technology to do the "dirty work." For example, Electronic Remittance Advice (ERA) allows for automated payment posting, reducing the human error associated with manual entry.
At Upfront Operations, we're all about "game-changing support." Whether it's setting up a professional digital presence or optimizing your sales operations, we believe in the power of specialized microservices. You can learn more about Upfront Operations and how we bring this same level of elite efficiency to our clients.
Artificial Intelligence is no longer a futuristic concept; it's a daily tool for efficient Revenue cycle management.
Patient collections are often the most uncomfortable part of the cycle. No one likes asking for money, especially in a care setting. However, price transparency is now a regulatory and ethical requirement.
The primary goal is to ensure the healthcare provider receives accurate and timely reimbursement for services rendered. By optimizing every step from registration to final payment, RCM ensures the financial stability of the practice, allowing clinicians to focus on patient care rather than chasing checks. It also fosters payer-provider transparency, reducing the "friction" that leads to long payment delays.
RCM is often the first and last touchpoint a patient has with your practice. Financial transparency reduces the stress of "surprise bills," which is a major driver of patient dissatisfaction. When a practice supports equitable access through clear financial conversations and assistance programs, it moves the patient into the "Satisfied Customer" phase, increasing loyalty and the likelihood of timely payment.
Revenue cycle management is a complex, never-ending loop that requires constant vigilance. From navigating payer variability and evolving regulations to managing staff turnover, the challenges are real. However, by focusing on revenue integrity and leveraging the right KPIs and technology, any practice can achieve financial health.
At Upfront Operations, we understand that managing the "back office" can be overwhelming. That’s why we offer on-demand microservices to take the weight off your shoulders. Whether you need a business email setup to look professional for your New York clients, a new website to attract patients, or fractional sales operations to help your health-tech company scale, we are here to provide elite support with unstoppable momentum.
Ready to stop leaving money on the table? Explore more info about our services and let us help you build an operation that never sleeps.